|
Today, more children in Australia and around the world are developing short-sightedness (myopia) and from an earlier age. But thankfully we can now slow childhood short-sightedness progression and help prevent high myopia with effective treatments which weren't available a generation ago. As one of Melbourne's leading myopia control optometrists, many of the kids who come to our practice have parents who have high myopia themselves (some as high as -10.00 to -16.00) and understandably very concerned about their children's eyesight growing up. Myopia is, at least in part, a hereditary condition. Children with both parents having myopia have a 6 times risk of developing short-sightedness, and more severely. So at what age can we start myopia treatment for your child? There is no age requirement for starting myopia control treatment. We recommend starting treatment as soon as we have identified that your child is at high risk of developing high myopia (> -6.00) in the future. This reduces your child's lifelong risks of glaucoma, retinal detachment and myopic macular degeneration — diseases with a potential for blindness. Here at Eyecare Concepts, we have prescribed myopia control treatment for children as young as 3 years of age. Which children are in the high-risk category for myopia? Younger children, those at age 7 or under at the time of being first diagnosed with short-sightedness, are at highest risk. And the younger the child, the greater the risk — there is more time for the eyeball to grow and elongate as the child grows through the years of adolescence and puberty. We also analyse individual data for each child to determine their rate of myopia progression per year. A documented myopia increase of -1.00 or more in a 12 month period is considered rapid progression that should be treated. Is it possible to predict if a child will become short-sighted? Yes, it is possible to make predictions based on a child's current level of refractive error. Generally, across the population, a normal 3 year old child should be long-sighted by around +2,00, a 4 year old around +1.50 and a 6 year old around +1.00. Long-sightedness acts as a buffer to prevent short-sightedness in a normally-developing eye. If we identify that your child is less long-sighted than is normal for his or her age, your child has a greater risk of developing short-sightedness and needs to be monitored more closely. For example, a child who is only +0.25 long-sighted at age 4 has a very high myopia risk, especially if this child has other risk factors such as genetics. There are specific tests we do to accurately measure the refractive status of a young child. Can we prevent the onset of myopia with treatment? Recent studies have shown that spending more time outdoors (for at least 90 minutes a day) has a protective effect on the eye and can prevent or delay the onset of childhood short-sightedness. For children who are not yet short-sighted but are at risk, we prescribe an increase in outdoor time as a preventative measure. Low-dose atropine treatment is highly effective in slowing progression once a child is already short-sighted, but there is little clinical data at present on its effect for myopia prevention in children with normal eyesight. There is some suggestion that it can indeed prevent myopia onset. We would assess the possibility of prescribing low-dose atropine for myopia prevention in a child without myopia on a case-by-case basis by weighing up the potential benefits vs risks. Certain glasses may help children who have difficulties with near focusing and eyestrain that can increase their risk of myopia development. Binocular vision testing is part of the comprehensive children's vision assessment in our clinic to identify these at-risk children. If you have questions about myopia control treatments for your child, please contact our clinic. EYECARE CONCEPTS · THE MYOPIA CLINIC
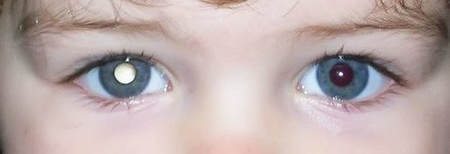
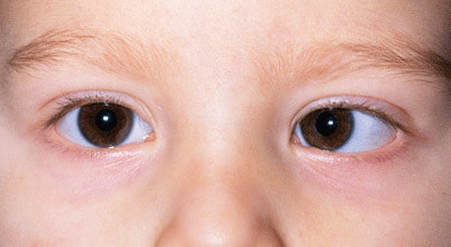
MELBOURNE MYOPIA CONTROL OPTOMETRIST — KEW · KEW EAST · BALWYN All children should have their first eye test by an optometrist by the age of 3, and reviewed at least every year as they grow up.Good vision is vital for a child's growth and development, as most of what a young child learns about the world comes from their eyesight. Poor eyesight in kids, which they often are not aware of and do not complain about, can lead to behavioural issues, delayed social development and learning difficulties. While young children will have an eyesight screening test by the Maturnal & Child Health Service, these are typically very basic tests that may not reliably detect all vision issues. It is recommended that all children by the age of 3 have a comprehensive, professional vision and eye health assessment by a children's optometrist. HOW WE TEST YOUNGER KIDS' EYES At Eyecare Concepts, our paediatric optometrist routinely tests children as young as 2, and sometimes even younger. Children's eye tests are different from adults' eye tests, requiring a different set of skills and equipment. We tailor the eye test to your child's age, maturity level and responses. Many tests are objective, meaning we can obtain reliable results without necessarily needing a response from your child. Our kids-friendly clinic is equipped to test younger children's eyes more thoroughly than most general retail optometrists. We schedule 40 minutes for a children's vision assessment to allow ample time for children to settle and feel comfortable in our spacious consulting room. As it may be their first eye test, some children can be understandably a little nervous and anxious in new surroundings. Our aim is to make their eye test a fun and enjoyable experience, and as always, to provide the best eye care. In a typical eye test for a preschool child, we check their eyesight with our children's eye test chart (picture matching), measure any potential focusing issues with a special light or a computerised vision tester, check eye movements, look for signs of a turned eye or lazy eye, check stereo acuity (ability to see 3D), colour vision, and the health of the front and back of their eyes. Eye drops are sometimes required to allow us to check the child's vision status and eye health in more detail. KIDS' VISION PROBLEMS Young children can have myopia (short-sightedness), hyperopia (long-sightedness) and astigmatism (irregularly shaped eye) just like adults can. Many eye problems actually run in families, so if you have an eye condition there's a good chance that your child may also have it, or may develop it. It is of even greater importance that vision problems are detected early in children, as delayed treatment can potentially affect their vision for life. By having their first eye test before the age of 3, we have a baseline to compare and monitor any vision changes as they grow up. It also allows for us to predict when your child may begin to have eyesight problems and to make recommendations to help prevent or delay the onset of these problems. Children who are already short-sighted before 5 have a very high risk of developing high myopia, which has lifelong eye health implications. More Australian children today are becoming short-sighted, and at an earlier age, than before. We have a specialised myopia treatment program to control childhood eyesight deterioration that occurs with progressive myopia. Our optometrist has successfully treated many young children to slow down their rate of myopia progression. Below are two other examples of childhood eye problems that require urgent attention: WHITE REFLEX If you come across a photo of your child with a white reflex in one eye (like the image below), you should seek medical attention immediately as it may be a very serious problem. An opacity in the eye, a cataract, retinal detachment or a retinal tumour (retinoblastoma) can cause this white reflex phenomenon. Retinoblastoma is a rare eye cancer found in younger children (usually before age of 5, and more commonly before 2) that, if not detected and treated, may spread and become life-threatening. EYES NOT STRAIGHT If you have noticed that your child's eyes are not straight, whether it's subtle or obvious, sometimes or all the time, your child needs a detailed eye examination. A turned eye or strabismus (also called a 'squint') may involve one eye turning inwards or outwards relative to the other eye. It is caused by a misalignment, imbalance or weakness in the muscles that move the eyes. Strabismus occurs in about 2-4% of all children. Many cases of strabismus are caused by a high degree of long-sightedness (hyperopia) in one eye and can be corrected with glasses without needing surgery. Failing to diagnose and treat strabismus from an early age can lead to the development of amblyopia ('lazy eye') which is permanent vision loss in one eye that cannot be treated or corrected in adulthood. Amblyopia needs to be treated early — typically before age of 8 — for best results. We can treat childhood amblyopia with glasses correction, patching and atropine eye drop therapy. Where necessary we can also refer your child to a paediatric ophthalmologist (an eye specialist) for further assessment and management. If you have a concern about your child's eyes, book an appointment to see our paediatric optometrist as soon as possible. We can test children as young as 6 months with advanced technology specific for assessing children's eyes. EYECARE CONCEPTS
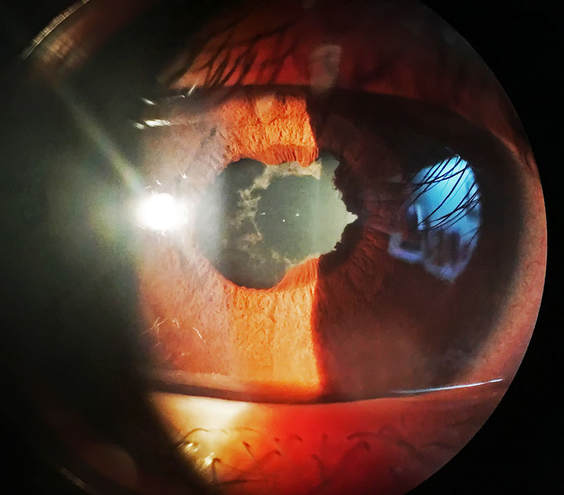
FAMILY & CHILDREN'S OPTOMETRIST — KEW EAST, MELBOURNE A young lady in her 20s came to see us recently after having a sore red eye and blurred vision for about 5 days. She had been using the common over-the-counter antibiotic eye drop Chlorsig, typically used for a mild case of bacterial conjunctivitis (pink eye). This was the appearance of her eye on presentation: This young lady did not have conjunctivitis; she had a classic case of an eye condition called anterior uveitis, or iritis. It is an inflammatory condition of her iris, the coloured part of the eye that controls the pupil. It is a relatively uncommon condition that can affect a person of any age, typically a young to middle-age person. Symptoms usually include increased sensitivity to light (photophobia), eye pain or ache, redness in the eye, blurred vision and one pupil appearing smaller than the other.
Optometrists can diagnose anterior uveitis, and differentiate it from other kinds of pink eyes, by detailed examination of the eye with our slit lamp microscope. The necessary treatment for this condition is immediate and rapid control of the inflammation with a intense course of steroid eye drops (prednisolone acetate — Pred Forte) — typically every 15 minutes in the first 6 hours, then hourly dosing while awake, and reviewed the following day. A strong pupil dilation eye drop (eg. atropine) is also used to keep the pupil enlarged to prevent the inflammed iris from sticking to the front of the eye's natural lens (posterior synechiae). In this case as the iris had already adhered to the lens she had some permanent damage to her iris and pigment spots left on her lens. If this kind of eye inflammation is left untreated or not properly managed, vision loss and glaucoma (high eye pressures causing optic nerve damage) can result. With our treatment of strong steroid eye drops and pupil dilation drops she had relief from her eye pain within a short period of time. And at her next-day follow up the inflammation and redness had already subsided significantly with treatment. After continuing with treatment and allowing the inflammation to completely resolve, we referred her to see her GP for blood tests as anterior uveitis is a eye condition that has a strong association with other systemic inflammatory or autoimmune disorders. The take-home message from this case is that if you have a concern about your eye, please see an eye care professional who can make a sound clinical diagnosis and give you the treatment you need right away. Not all pink eyes are common conjunctivitis — if you have a painful (more than just an irritation) red or pink eye, light sensitivity or blurred vision you should see either a therapeutically-endorsed optometrist (an optometrist who is trained and qualified to prescribe medicines) or an ophthalmologist (eye specialist) without delay. And if you've been using an antibiotic eye drop such as Chlorsig for a pink eye but it doesn't show improvement, please seek further opinion for your eye promptly. For an after hours emergency or if you are unable to find a suitable eye care practitioner, the Royal Victorian Eye & Ear Hospital in East Melbourne would be the place to go. EYECARE CONCEPTS — THERAPEUTIC OPTOMETRIST — KEW EAST, MELBOURNE |
AuthorPhilip Cheng - B.Optom (Melb) Ocular Therapeutics (GCOT). Optometrist at Eyecare Concepts Kew East, Melbourne. An experienced eye care & contact lens practitioner with expertise in myopia control & orthokeratology. Archives
August 2018
Categories
All
|
Eyecare Concepts | The Myopia Clinic © 2017-23
KEW EAST | MELBOURNE
KEW EAST | MELBOURNE











 RSS Feed
RSS Feed